Pain is not a deluxe issue in emergency situation care, it is the presenting signs and symptom that forms every choice you make in the first minutes. Treat pain efficiently and you get trust fund, enhance evaluation accuracy, and frequently prevent complications. Obtain it wrong and the whole experience tilts. The certified unit PUAEME008 Provide discomfort monitoring sits directly in that room. It gives paramedics, first responders, occasion medics, and medical support staff a functional, defensible framework to reduce pain securely in unrestrained environments.
I have actually shown and executed this unit throughout rescue solutions and remote facilities, and the very same styles repeat: the protocols look simple theoretically, yet actual scenes are messy. You have to safeguard a line of vision to what matters most, scoot without reducing corners, and file as if an auditor rides in the jump seat. This write-up breaks down what the training covers, why it is structured the method it is, and how it attaches to wider pain administration courses for nurses and physio therapists who support prehospital groups or run in urgent-care settings.
Where PUAEME008 Suits the Training Landscape
The PUAEME008 give discomfort monitoring system is normally embedded within public safety and security and emergency response credentials. You will certainly see it paired with standard life support, oxygen therapy, and analgesia components in certificate-level plans designed for functional responders. It does not claim to be a thorough discomfort fellowship, and that is proper. The focus is secure, prompt analgesia with limited sources, commonly prior to a conclusive diagnosis exists.
For clinicians originating from medical facilities, this can seem like an action down in pharmacology deepness, however in truth it is a step up in threat administration. Emergency situation discomfort management on an aesthetic at 3 a.m. differs from an ED cubicle with full tracking and pharmacy gain access to. The system calibrates decisions to that field truth: short evaluations, repeat monitorings, conventional application, and solid focus to contraindications that are easy to miss when the wind is up and the patient is pale and sweating.
This unit can sit together with a certification course in pain monitoring used to multidisciplinary team. The difference is emphasis. A pain monitoring certification program in a healthcare facility system studies multimodal and persistent structures. PUAEME008 supports severe, usually terrible, presentations with short half-life choices, straightforward delivery systems, and distinct documentation.
What the Unit In fact Covers
Training suppliers vary in delivery, however the core end results remain consistent. You discover to examine discomfort rapidly using courses for physiotherapists in pain management common scales, to select appropriate analgesic pathways within your scope, to carry out, monitor, and afterwards reassess. You also learn to intensify when the picture does not fit or pain continues to be uncontrolled.
Typical range includes:
- Scene-based assessment and differential framing of pain in the very first 5 mins: trauma versus clinical, warnings that imply time-critical pathology, and how pain itself can mask or mimic severity. Analgesic options lined up with the responder's scope and jurisdiction. The familiar trio is inhaled methoxyflurane where allowed, dental or transmucosal agents, and basic parenteral options for those endorsed. Some solutions include intranasal opioids or ketamine under particular protocols. The device shows indicator thresholds and stop rules. Non-pharmacological methods like placing, immobilisation, splinting, ice or heat when suitable, interruption, and assisted breathing. In busy changes these get neglected, yet they usually reduced discomfort scores by two or 3 points prior to any kind of drug takes effect. Monitoring for effectiveness and damaging impacts. You discover to cycle monitorings at defined periods and to associate subjective discomfort ratings with unbiased pens: breathing rate, end-tidal CO2 where offered, mental condition, perfusion, and movement. Communication and permission. The system stresses explaining options clearly, acquiring notified authorization or proceeding under indicated authorization where ability suffers, and recording the reasoning in clear language.
The evaluation is sensible. You go through circumstances that vary from an ankle fracture at a sports occasion to a baffled older grown-up with stomach pain. Teachers will watch how you verbalise risk, how rapidly you see altering vitals, and whether you ask for help early. Paper expertise helps, however it is the behaviors under time pressure that pass or fail you.
Why Emergency situation Pain Management Demands a Different Lens
In controlled environments it is easy to develop an excellent discomfort ladder. Visible, priorities change. The most common mistake I see is incorrect accuracy, a tendency to look for the optimal medical diagnosis prior to supplying first-line alleviation. In a roadside crash with an obvious defect, awaiting a full differential misreads. Pain itself drives tachycardia and hyperventilation, intensifies anxiety, and obstructs purposeful evaluation. Analgesia becomes a diagnostic device. As the discomfort goes down, you can palpate, reposition, and examination operate more accurately.
The second distinction is permission under unpredictability. The individual is often nervous, hypoxic, or intoxicated. You still aim for approval, however you mount it crisply. "I can use a fast-acting breathed in discomfort medication. It disappears quickly, some people really feel lightheaded. Would you like that while we splint your leg?" Then you pause, see their eyes, listen for the yes. Excellent training instructs this cadence.
Finally, the system appreciates that -responders often function alone or as a set without a physician on the radio. Methods need to be clear, not based on extensive consults. If the policy allows methoxyflurane approximately a specified maximum, you discover to dosage, monitor, and stop within those borders. If intranasal fentanyl is consisted of, you discover precise quantities per nostril, spacing, and saturation limits that trigger an adjustment of plan.
The Pharmacology You Actually Use
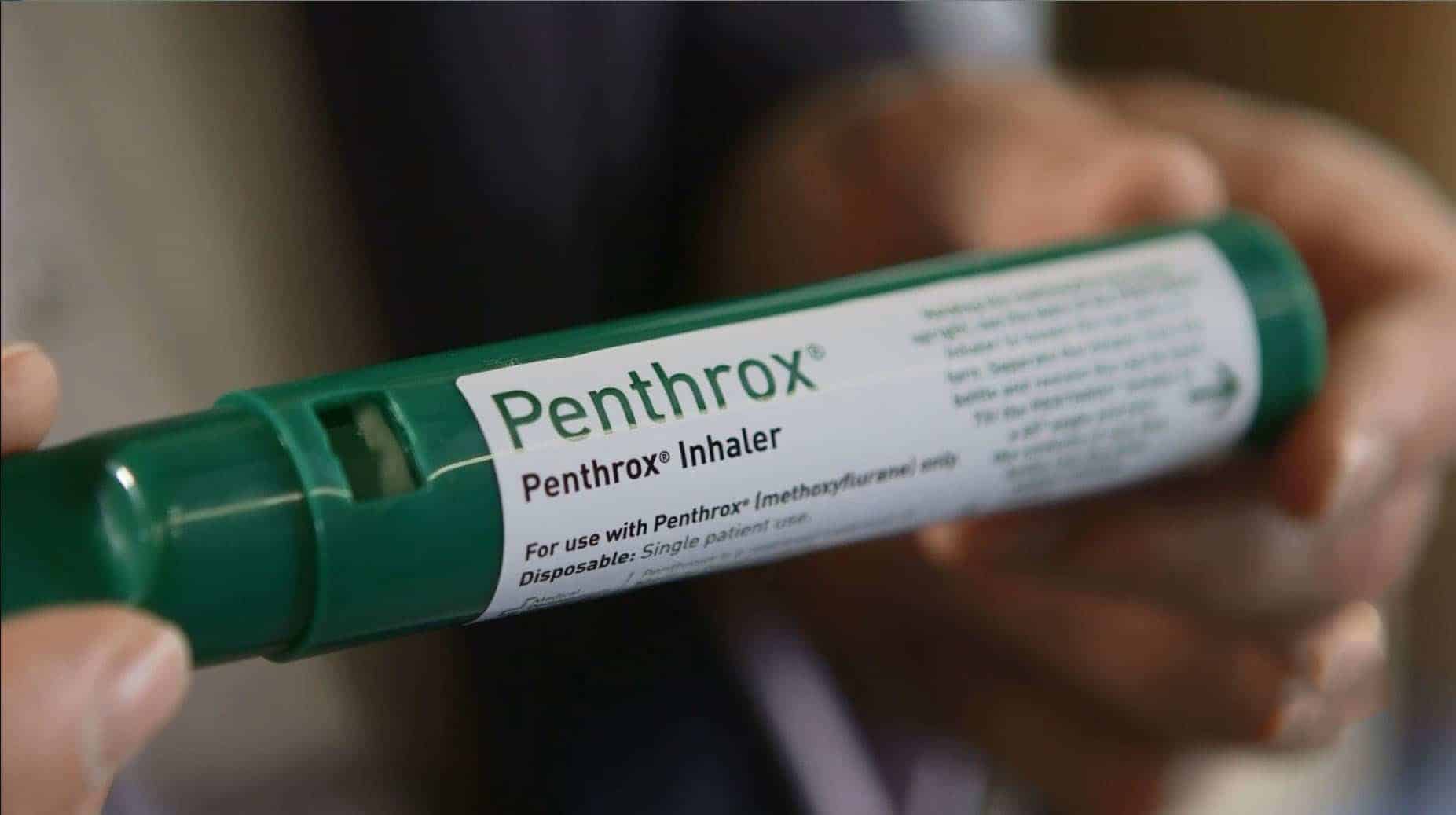
Most PUAEME008-aligned programs prioritise representatives that are portable, fast-onset, and very easy to titrate. Precise formularies depend on the service, but numerous patterns show up once more and again.

Methoxyflurane, where readily available, is a field workhorse. It is breathed in, self-administered with coaching, and it enables a safeguarded sort of self-titration. The training stresses guidance, limiting total dose, and identifying when a person's strategy falls short because of frustration or tiredness. It likewise educates environmental security. The smell is distinctive, and in improperly ventilated rooms suppliers can really feel dull or headachy. Fracture a window, step outside if functional, and turn jobs so the exact same staff member does not hover by the mouthpiece for twenty minutes.
Intranasal opioids, generally fentanyl, load the space when inhaled alternatives are contraindicated or inadequate. The intranasal path avoids needle stick threat and relocates quickly via vascular nasal tissue. You discover to divide the dosage in between nostrils, adjust for age and frailty, and pay callous focus to respiratory tract tone once discomfort decreases. You practice what to do if respiratory system rate slides below limits, when to reposition, when to add oxygen, and when to reverse.
Ketamine, in some extended-scope services, gains its location for stressful pain that resists other agents, particularly when hypotension makes opioids risky. The unit does not transform -responders into anaesthetists. It insists on accurate application, clear contraindications like psychosis, and durable surveillance. The advantage is immense in remote setups where extrication and cot movement turn minutes right into an hour.
Paracetamol and non-steroidal anti-inflammatories do not get hold of headlines, yet their additive effect issues. Early enteral application together with fast-acting agents develops a bridge that holds with transport and handover. The device shows safe NSAID usage, kidney cautions, and gastric defense for older adults.
Non-Drug Methods That Matter Greater Than You Think
Every pain management course talks up non-pharmacological techniques. In emergency situation treatment, those approaches are not "great to have." They are the very first treatment. Splinting an unstable ankle joint, extra padding a backboard stress factor, raising an arm or leg to reduce pain, and orchestrating a tranquil atmosphere all change the patient's experience before a solitary dosage. I frequently ask students to attempt their discomfort scale again after appropriate positioning. The number regularly visits 2. That drop buys time and reduces overall medication load.
Guided breathing looks basic, but several responders hurry it. The method is to combine your breath and matter aloud, slow-moving enough to really feel uncomfortable. 5 seconds in, hold for a beat, 5 seconds out. Use your hand on their shoulder to set the tempo. After a min the jaw unclenches, and you can place the monitor leads without a fight.
Cold and warmth stay low-risk complements if you appreciate contraindications. Severe strains like ice bags in the first hours. Spasm-dominant low pain in the back may respond to warmth if there is no uncertainty of infection or trauma. The training shows you to ask short, targeted inquiries that reveal when an easy pack helps greater than a 2nd drug.
Documentation Is Part of the Therapy
I treat paperwork as part of analgesia. Excellent notes safeguard people, support scientific thinking, and speed ED decision-making. PUAEME008 drills a simple structure: standard pain rating, location and top quality descriptors, picked treatment with reasoning, the time of management, and a re-evaluation at specified intervals. If something feels incorrect, compose that down too. "Pain disproportionate to findings" is not a grievance, it is a diagnostic idea. It signifies compartment syndrome, vascular compromise, or occult stomach pathology.
Audit teams look for patterns. If every individual reports 10/10 pain before and 2/10 after, something is off. Learn to adjust the scale with clients. "Absolutely no is nothing in any way, ten is the worst pain you can envision. Where are you now?" Then anchor it with their own words. After treatment, request for the new number and what altered: "I can move my leg currently," or "it still stabs when I breathe." That subtlety helps the next clinician choice up the thread.
Safety Nets and Red Flags
The most skilled -responders bring 2 mental scripts: one for routine pain treatment and one for the exemptions. The unit clearly educates both. Red flags include unexpected severe headache unlike previous migraines, upper body pain with diaphoresis and radiation, stomach discomfort with safeguarding and hypotension, back pain with neurological deficits, and limb pain with pallor, pulselessness, or paraesthesia. Analgesia does not quit since a red flag exists, but lines of interaction open immediately. You inform receiving groups, reduce on-scene time, and maintain medicine selections conservative if they might mask vital signs.
Paediatric discomfort is its own world. Kids under-report or misreport, and distressed parents amplify or subdue cues. PUAEME008 utilizes age-appropriate scales like the Wong-Baker faces or empirical tools for preverbal toddlers. Dosing comes to be weight-based and margin for mistake narrows. I teach a practice of checking out doses from 2 independent resources on scene, such as a laminated card and a calculator app, to prevent basic transpositions.
Older grownups require a different care. Renal feature, polypharmacy, and cognitive baseline are frequently unknown. Low-and-slow dosing, longer observation, and very early consideration of non-opioid accessories decrease harm. If an individual with an autumn offers with moderate head strike and a typical test however takes anticoagulants, analgesia proceeds, but you promote for imaging and cautious handover.
How PUAEME008 Intersects With Other Disciplines
Pain management courses for nurses and pain administration courses for physiotherapists usually target subacute or persistent problems. Yet there is an efficient overlap with this emergency device. Registered nurses in urgent care and remote facilities manage first presentations when ambulance hold-ups stretch. A pain administration accreditation program that consists of severe triage skills, safe inhaled or intranasal alternatives, and monitoring enhances outcomes in those settings. Physiotherapists operating pitch-side or in industrial sites often come to be initial medical professionals to see injuries. Short training courses suffering administration that mirror PUAEME008 principles help them secure while waiting on transportation and connect successfully with getting teams.
For groups that extend duties, a common language matters. Settle on scale use, dosing language, and handover framework. I have seen multidisciplinary teams cut ten mins off scene time simply by straightening on who leads analgesia and who records. That is not trivia, it is the difference between a comfy person and one who arrives clenched and exhausted.
Choosing a Supplier and What Great Training Looks Like
A supply discomfort monitoring course need to leave you positive to act under stress, not simply to pass an analysis. Seek suppliers that instruct with realistic circumstances, actual tools you will use in the area, and trainers who have current functional experience. Ask exactly how they deal with adverse occasions. If the answer is "we cover that theoretically," maintain looking. You need to rehearse apnoea drills, throwing up throughout inhalation treatment, and handling agitation after ketamine, even if your service hardly ever deploys it.
Credentialing matters. Seek a pain management certificate aligned with your territory's criteria and recognised by your service. Paper alone is not nearly enough, however it opens doors. If your job arc includes innovative method roles, a pain monitoring accreditation that consists of broader pharmacology and multidisciplinary case studies matches PUAEME008. Ladder your training thoughtfully: begin with the emergency situation device, add a certificate course suffering monitoring for breadth, then target expert modules appropriate to your setting.
Practical Tips From the Field
These are the little actions that make huge distinctions over years of practice.
- Prepare your analgesia set like a cockpit, with the same design every change. Muscle memory under stress prevents dosing mistakes and rates shipment. If you share kits across teams, standardise the format and tag syringes and atomisers clearly.
Triage your conversations. Individuals suffering hear about one sentence in 3. Lead with what issues: "I can lower your pain now. Here is exactly how it functions." Then deal with permission, risks, and next action in short, concrete expressions. Check understanding with a concern that demands an option, not a yes/no nod.
Use time checkpoints. In my crews we call the first 5-minute reassessment out loud and document it within one minute. That tiny routine improves both safety and handover quality.
Treat nausea or vomiting quickly. Throwing up weakens client trust and makes complex airway safety. If your procedures allow, match analgesia with an antiemetic for high-risk situations: motion in the rear of a gear, terrible discomfort, or prior history.
Hand over the client with a discomfort story. "Showed up to 8/10 discomfort in the ideal hip, provided breathed in analgesia with a decrease to 4/10, then intranasal opioid with a drop to 2/10. Stable vitals throughout. Pain spikes to 6/10 when we roll. Splinted and cushioned." This string overviews the obtaining group to proceed the strategy as opposed to reactivate from zero.
Assessment and Proficiency: What to Expect on the Day
The sensible analysis in PUAEME008 normally unravels across a couple of situations and a brief written part. For the circumstances, assessors enjoy your flow greater than your memory of minute information. They wish to see you scan for danger, recognize and measure pain, select a treatment within extent, and then follow up with tracking and documentation.
If you blank on a dose, say so, locate the recommendation, and proceed correctly. That makes more trust than presuming. If the individual's discomfort does not shift, you escalate within the procedure and ask for clinical guidance if suggested. They will likely introduce a curveball: nausea or vomiting, a drop in saturation after opioid, or a parent who declines a treatment for a kid. Keep calm, demonstrate choices, and document deviations.
For the created portion, expect short-answer concerns on authorization, contraindications, and negative effects. The objective is not to trap you, yet to verify that you comprehend why the protocol says what it says.
Connecting PUAEME008 to Job Growth
Many responders view pain management training as a checkbox. That offers it brief. Skills in analgesia correlates with total scene leadership. You interact better because you relieve experiencing early. People talk with you, you gather more clear backgrounds, and your vitals are a lot more dependable due to the fact that they are not misshaped by distress. Supervisors notice. When positions open for group leaders or clinical support policemans, the responders who take care of pain cleanly typically rise.
For nurses, a discomfort administration qualification training course that includes prehospital components opens up urgent-care roles and occasion medication job. For physio therapists, adding emergency pain monitoring skills anchors your position on sporting activities medicine groups and work-related health and wellness programs. A pain management certificate does not replace professional degrees, but it widens your range safely.
A Note on Ethics and Equity
Pain is not dispersed evenly throughout populations. Cultural expression of discomfort varies, and implicit bias forms exactly how clinicians react. The most effective pain management training programs resolve this head-on. You find out to use regular scales, not gut feelings based on who "looks" hurting. You discover to ask open questions, and to validate reported pain even when it surpasses your expectation for the visible pain management training certification injury. In remote and Native areas, trust can be slim. Bringing prompt analgesia without rubbing constructs bridges. That matters more than most methods admit.
Final Ideas: Make Discomfort Relief a Reliable Habit
PUAEME008 codifies practices that experienced clinicians currently technique. Analyze rapidly, deal with early, combine non-drug and medicine procedures, screen closely, and record without drama. It provides you a framework that holds when adrenaline spikes or when tiredness dulls judgment at 4 a.m. It also develops a common language across groups. If you operate in emergency situation treatment and you do not yet hold this device, it belongs on your listing of discomfort management training programs to finish. If you currently hold it, revisit the skills every year. Bring an associate, swap duties, and audit each other's charts for a shift. The patients will certainly not remember your certificate number. They will keep in mind being heard, being assisted, and being able to take a breath without bracing every rib. That is the heart of emergency discomfort management.
For those building wider pathways, mix this training with a discomfort monitoring certificate course that checks out multimodal strategies, pharmacovigilance, and communication across disciplines. Registered nurses who anticipate to triage and stabilise need to consider pain monitoring training for nurses that consists of intranasal analgesia, age-specific ranges, and rise protocols. Clinicians in sporting activities and bone and joint treatment can benefit from discomfort administration programs for physio therapists that mirror severe treatment realities, including splinting and event-side decision-making. Whether you choose a short training course in pain monitoring or a more thorough pain administration qualification course, allow the PUAEME008 frame of mind support your method: relieve pain early, safely, and with enough humility to adjust as brand-new details arrives.